Introduction
Facelift surgery is one of the most frequently performed aesthetic procedures in the United States, with nearly 70,000 cases reported in 2019 alone, placing it among the top six cosmetic operations. While most patients enjoy a smooth recovery, short‑term issues such as hematoma, seroma, bruising, and temporary numbness are common, and long‑term concerns can include scar visibility, nerve weakness, skin necrosis, or uneven results. Because complications are often linked to modifiable factors—blood pressure, smoking, medication use, and body‑mass index—thorough pre‑operative assessment and targeted risk‑reduction strategies are essential. Proper patient selection, meticulous surgical technique, and strict adherence to postoperative instructions together dramatically lower the likelihood of adverse outcomes.
Immediate Post‑Operative Effects and Common Complications
| Effect / Complication | Typical Onset | Typical Duration | Common Management |
|---|---|---|---|
| Swelling (edema) | 0‑48 hrs, peaks 48‑72 hrs | 1‑2 weeks (resolves) | Head elevation, compression, analgesics |
| Bruising | 0‑48 hrs, peaks 48‑72 hrs | 1‑2 weeks | Cold compress, time |
| Tightness / soreness | Immediate | Days‑to‑weeks | Prescribed analgesics, gentle massage |
| Numbness / tingling | Immediate (nerve stretch) | 3‑6 months (usually resolves) | Observation, neuropathic meds if needed |
| Hematoma | Within 24 hrs | Immediate concern, may persist if untreated | Needle aspiration or OR evacuation, compression |
| Seroma | 1‑3 days | Days‑to‑weeks if symptomatic | Drainage, compression |
| Infection | Rare (<1 %) | Days‑to‑weeks if develops | Antibiotics, wound care |
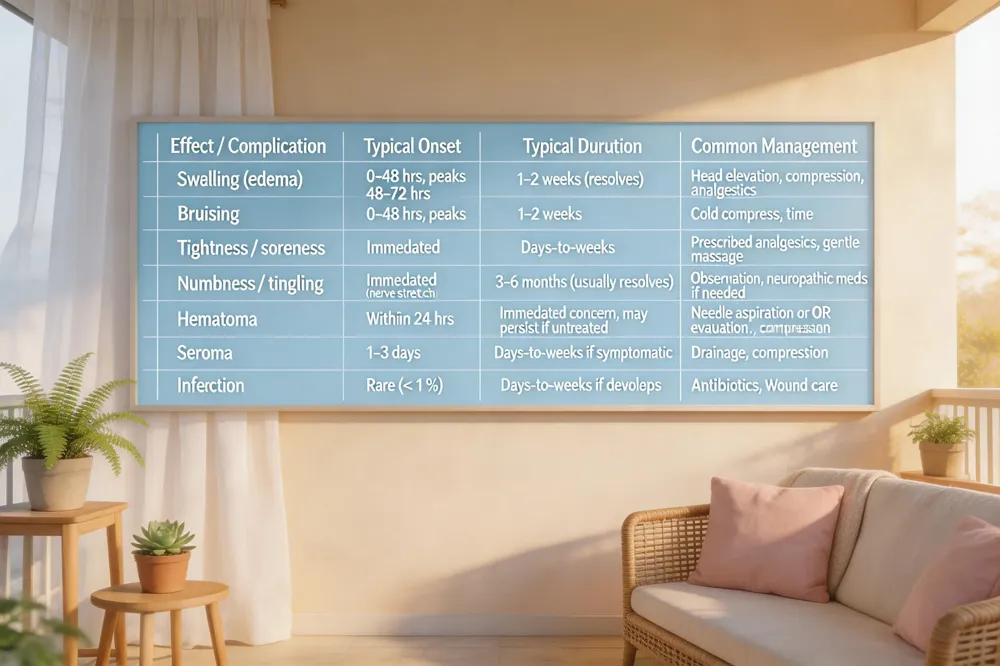 Swelling, bruising and mild discomfort are the most frequent early‑effects after a facelift. Edema typically peaks within the first 48‑72 hours and then recedes over one to two weeks, while bruising fades in a similar time‑frame. Patients often report a sensation of tightness or soreness that is well‑controlled with prescribed analgesics. Temporary numbness or tingling is common because facial nerves are gently stretched or irritated during dissection; this sensory change usually resolves as the nerves heal, often within 3‑6 months. The single most common serious complication is a postoperative hematoma—a collection of blood under the skin that usually appears within the first 24 hours. Hematomas can cause swelling, pressure and bruising and, if untreated, may compromise skin perfusion; management may involve needle aspiration or a brief return to the operating room for evacuation. Small fluid collections (seromas) are less frequent and are managed with drainage if symptomatic. Infection is rare (<1 %) but must be addressed promptly when warmth, redness, pain or fever develop.
Swelling, bruising and mild discomfort are the most frequent early‑effects after a facelift. Edema typically peaks within the first 48‑72 hours and then recedes over one to two weeks, while bruising fades in a similar time‑frame. Patients often report a sensation of tightness or soreness that is well‑controlled with prescribed analgesics. Temporary numbness or tingling is common because facial nerves are gently stretched or irritated during dissection; this sensory change usually resolves as the nerves heal, often within 3‑6 months. The single most common serious complication is a postoperative hematoma—a collection of blood under the skin that usually appears within the first 24 hours. Hematomas can cause swelling, pressure and bruising and, if untreated, may compromise skin perfusion; management may involve needle aspiration or a brief return to the operating room for evacuation. Small fluid collections (seromas) are less frequent and are managed with drainage if symptomatic. Infection is rare (<1 %) but must be addressed promptly when warmth, redness, pain or fever develop.
Hematoma: Why It Happens and How It’s Managed
| Factor | Details | Prevention / Management |
|---|---|---|
| Vessel disruption | Dissection of facial vessels | Meticulous hemostasis, careful tissue handling |
| Elevated BP (>150 mm Hg) | Hypertension spikes post‑op | Peri‑op BP control (clonidine, labetalol, hydralazine) |
| Epinephrine rebound | Vasoconstriction wears off | Limit epinephrine in tumescence, second‑look closure |
| BMI > 25, smoking, male sex | Higher risk profile | Optimize health pre‑op, smoking cessation |
| Small hematoma | Minor collection | Head elevation, compression dressings |
| Large hematoma | Significant collection | Fine‑needle aspiration or incision drainage; OR evacuation if persistent |
| Seroma | Fluid collection | Drainage if symptomatic, compression |
 Post‑operative hematoma after a facelift results from bleeding that accumulates under the skin, usually within the first 24‑48 hours. Disruption of facial vessels during dissection, combined with high systolic blood pressure (>150 mm Hg) or rebound bleeding from epinephrine‑containing tumescence, creates a space where blood can pool.
Post‑operative hematoma after a facelift results from bleeding that accumulates under the skin, usually within the first 24‑48 hours. Disruption of facial vessels during dissection, combined with high systolic blood pressure (>150 mm Hg) or rebound bleeding from epinephrine‑containing tumescence, creates a space where blood can pool.
Effective prevention starts with strict peri‑operative blood‑pressure control—pre‑op clonidine and intra‑op labetalol or hydralazine are commonly used, especially in men, smokers, or patients with BMI > 25. Eliminating epinephrine from the tumescence solution and employing a “second‑look closure” (delaying final skin closure until the opposite side and submental work are finished) allow vasoconstriction to wear off, minimizing rebound bleeding.
If a hematoma forms, management depends on size and symptoms. Small collections may be observed with head elevation and compression dressings. Larger or painful hematomas are typically drained by fine‑needle aspiration or a small incision; persistent or expanding collections require operative evacuation and hemostasis. Early intervention, compression, and a brief course of antibiotics or anti‑inflammatories help prevent contour distortion and promote rapid recovery.
Safety for Older Adults and Recovery Best Practices
| Consideration | Recommendation | Rationale |
|---|---|---|
| Physiologic age assessment | Evaluate cardiac, pulmonary, healing capacity | Chronological age > 70 not limiting if health good |
| Procedure selection | Mini‑lift or selective fat redistribution for septuagenarians | Reduces operative time, blood loss, anesthesia exposure |
| Anesthesia | Local anesthesia or limited sedation | Lowers systemic risk |
| Post‑op activity | Gentle movement, avoid heavy lifting for 2‑3 weeks | Prevents clots, strain on sutures |
| Lifestyle | Quit smoking, stay hydrated, protein‑rich diet | Enhances tissue healing, reduces infection |
| Follow‑up | Attend all scheduled visits (day‑1, week‑1, month‑1, etc.) | Early detection of complications |
| Pain management | Use prescribed meds as directed | Controls discomfort, avoids over‑exertion |
 Facelift surgery can be performed safely on patients over 70 when the surgeon evaluates physiologic, chronological, and legal age, and that lung function, blood pressure, smoking status, and overall healing capacity. For septuagenarians with good health, a mini‑lift or selective fat redistribution often provides natural rejuvenation while limiting operative time, blood loss, and anesthesia exposure.
Facelift surgery can be performed safely on patients over 70 when the surgeon evaluates physiologic, chronological, and legal age, and that lung function, blood pressure, smoking status, and overall healing capacity. For septuagenarians with good health, a mini‑lift or selective fat redistribution often provides natural rejuvenation while limiting operative time, blood loss, and anesthesia exposure.
Is a facelift safe for patients over 70? Yes—a facelift can be safe for patients over 70 when they are in good overall health and have realistic expectations. Surgeons focus on the patient’s physiologic age, checking cardiac and lung function, smoking status, and healing ability rather than using chronological age alone. Modern techniques often use local anesthesia or limited‑sedation and less‑invasive tissue‑tightening methods, which reduce operative risk and shorten recovery. A board‑certified facial surgeon will tailor the plan—sometimes opting for a smaller “mini‑lift” or selective fat redistribution—to match the individual’s skin elasticity and bone structure. With proper pre‑operative screening and post‑operative support, most healthy septuagenarians experience safe outcomes and natural‑looking results.
How can patients minimize the risk of complications during recovery? Patients can minimize complications by strictly following their surgeon’s post‑operative instructions, including wound‑care protocols and activity restrictions. Maintaining a healthy lifestyle—quitting smoking, staying well‑hydrated, eating a balanced diet rich in protein and vitamins—supports tissue healing and reduces infection risk. Attending all scheduled follow‑up appointments allows the care team to monitor progress and intervene early if problems arise. Gentle, surgeon‑approved movement and gradual return to normal activities help prevent blood clots, excessive swelling, and strain on healing tissues. Finally, managing pain with prescribed medications as directed and avoiding over‑exertion ensures a smoother, safer recovery.
Deep‑Plane vs Traditional Facelift: Technique and Longevity
| Aspect | Deep‑plane Facelift | Traditional (SMAS) Facelift |
|---|---|---|
| Plane of dissection | Below SMAS, includes deep ligaments | At SMAS level only |
| Structures moved | Muscles, fat pads, connective tissue as unit | SMAS and skin only |
| Typical candidates | Moderate‑to‑advanced laxity, desire for long‑term results | Younger patients, milder aging |
| Longevity | 10‑15 years+ | 7‑10 years |
| Recovery | More swelling, longer recovery (2‑3 weeks) | Faster healing, less discomfort |
| Nerve risk | Modest increase in buccal‑branch irritation | Higher temporary weakness with high‑lateral SMAS lifts |
| Complexity | Technically demanding | Generally less complex |
 A deep‑plane facelift works beneath the SMAS (superficial muscular‑aponeurotic system) layer, releasing deep retaining ligaments and moving the facial muscles, fat pads, and connective tissue as a single unit. In contrast, a traditional (or SMAS) facelift repositions only the SMAS and skin, tightening the superficial layer. Because the deep‑plane technique targets deeper structures, it can lift the mid‑face, cheeks, jawline, and neck together, delivering more dramatic, natural‑looking rejuvenation that often endures 10‑15 years or more. The traditional facelift primarily improves lower‑face sagging and jowls, with a shorter durability of about 7‑10 years. Deep‑plane surgery is technically more demanding, usually involving more swelling and a longer recovery, whereas the SMAS lift generally heals faster with less discomfort. Nerve‑injury risk differs slightly: high‑lateral SMAS and composite lifts have higher odds of temporary facial‑nerve weakness than SMAS plication, while deep‑plane work carries a modest increase in buccal‑branch irritation. Overall, a deep‑plane facelift provides greater longevity for patients with moderate‑to‑advanced laxity, while younger patients with milder aging often opt for the traditional SMAS approach.
A deep‑plane facelift works beneath the SMAS (superficial muscular‑aponeurotic system) layer, releasing deep retaining ligaments and moving the facial muscles, fat pads, and connective tissue as a single unit. In contrast, a traditional (or SMAS) facelift repositions only the SMAS and skin, tightening the superficial layer. Because the deep‑plane technique targets deeper structures, it can lift the mid‑face, cheeks, jawline, and neck together, delivering more dramatic, natural‑looking rejuvenation that often endures 10‑15 years or more. The traditional facelift primarily improves lower‑face sagging and jowls, with a shorter durability of about 7‑10 years. Deep‑plane surgery is technically more demanding, usually involving more swelling and a longer recovery, whereas the SMAS lift generally heals faster with less discomfort. Nerve‑injury risk differs slightly: high‑lateral SMAS and composite lifts have higher odds of temporary facial‑nerve weakness than SMAS plication, while deep‑plane work carries a modest increase in buccal‑branch irritation. Overall, a deep‑plane facelift provides greater longevity for patients with moderate‑to‑advanced laxity, while younger patients with milder aging often opt for the traditional SMAS approach.
Financial Aspects of Facelift Surgery in the Bay Area
| Procedure Type | Cost Range (USD) | Typical Inclusions |
|---|---|---|
| Mini‑facelift | $8,000 – $12,000 | Surgeon fee, facility, anesthesia |
| Traditional (full) facelift | $15,000 – $20,000 | Surgeon fee, facility, anesthesia |
| SMAS or Deep‑plane facelift | $20,000 – $25,000 | Surgeon fee, longer OR time, specialized skill |
| Ancillary procedures (neck lift, brow lift, fat transfer) | Additional $2,000 – $6,000 each | Depends on scope, facility, anesthesia |
| Financing | Often available via practice‑offered plans | Payments spread over months/years |
 In the San Francisco Bay Area, a facelift typically costs between $12,000 and $20,000, with the exact price depending on the surgeon’s experience, the facility, and anesthesia fees. Mini‑facelifts, which focus on the lower face and neck, often start around $8,000, while a full traditional facelift can run closer to $17,500 or higher. More extensive procedures such as a SMAS or deep‑plane facelift may reach $20,000–$25,000, reflecting the additional time and technical skill required. Most surgeons break the total price into three components: the surgeon’s fee, the operating‑room/facility charge, and anesthesia costs. Because insurance rarely covers cosmetic work, patients usually pay out‑of‑pocket or use financing options offered by the practice.
In the San Francisco Bay Area, a facelift typically costs between $12,000 and $20,000, with the exact price depending on the surgeon’s experience, the facility, and anesthesia fees. Mini‑facelifts, which focus on the lower face and neck, often start around $8,000, while a full traditional facelift can run closer to $17,500 or higher. More extensive procedures such as a SMAS or deep‑plane facelift may reach $20,000–$25,000, reflecting the additional time and technical skill required. Most surgeons break the total price into three components: the surgeon’s fee, the operating‑room/facility charge, and anesthesia costs. Because insurance rarely covers cosmetic work, patients usually pay out‑of‑pocket or use financing options offered by the practice.
Long‑Term Care, Side Effects, and Personalized Treatment Plans
| Aspect | Details | Recommendations |
|---|---|---|
| Scar maturation | 6‑12 months | Sunscreen, gentle scar massage, silicone sheets |
| Hyperpigmentation risk | UV exposure | Broad‑spectrum sunscreen, avoid peak sun |
| Permanent numbness / nerve weakness | Small % of patients | Counseling pre‑op, monitor, neuropathic meds if needed |
| Touch‑up procedures | Needed as natural aging resumes | Non‑surgical tightening, possible minor revisions |
| Personalized plan | Comprehensive facial assessment (skin, muscle, bone) | Tailor technique, incision placement, ancillary procedures |
| Follow‑up schedule | Day‑1 drain check, week‑1 bandage change, month‑1 suture removal, periodic up to 12 months | Early detection of issues, fine‑tuning results |
 Patients should expect scar tissue to mature over 6‑12 months; diligent sunscreen use and gentle scar massage reduce discoloration and elevation. UV exposure can cause hyperpigmentation or thinning, while a small percentage may experience permanent numbness, tingling, or mild facial nerve weakness. As natural aging returns, touch‑up procedures or non‑surgical tightening may be needed. Our center personalizes each facelift by first conducting a comprehensive facial assessment—skin quality, muscle tone, bone structure, and asymmetries—then selecting the optimal technique (full, mini, or lower) and incision placement to match the patient’s anatomy and goals. Ancillary procedures (neck lift, brow lift, fat transfer, laser resurfacing) are integrated when beneficial. A structured follow‑up schedule (day‑1 drain check, week‑1 bandage change, month‑1 suture removal, periodic visits up to 12 months) ensures early detection of complications and fine‑tuning of results.
Patients should expect scar tissue to mature over 6‑12 months; diligent sunscreen use and gentle scar massage reduce discoloration and elevation. UV exposure can cause hyperpigmentation or thinning, while a small percentage may experience permanent numbness, tingling, or mild facial nerve weakness. As natural aging returns, touch‑up procedures or non‑surgical tightening may be needed. Our center personalizes each facelift by first conducting a comprehensive facial assessment—skin quality, muscle tone, bone structure, and asymmetries—then selecting the optimal technique (full, mini, or lower) and incision placement to match the patient’s anatomy and goals. Ancillary procedures (neck lift, brow lift, fat transfer, laser resurfacing) are integrated when beneficial. A structured follow‑up schedule (day‑1 drain check, week‑1 bandage change, month‑1 suture removal, periodic visits up to 12 months) ensures early detection of complications and fine‑tuning of results.
Conclusion
Identifying and mitigating risks begins with a thorough pre‑operative assessment: control blood pressure, discontinue aspirin/NSAIDs, and stop smoking at least four weeks before surgery. Intra‑operative strategies such as strict hemodynamic monitoring, avoidance of epinephrine‑laden tumescence, and the use of quilting sutures or hemostatic nets dramatically lower hematoma rates. Selecting a board‑certified plastic surgeon who routinely operates in an accredited facility ensures adherence to sterile technique, prophylactic antibiotics, and vigilant anesthesia monitoring, all of which reduce infection, nerve injury, and thromboembolic events. Finally, patients who understand these precautions, ask detailed questions, and follow postoperative instructions are empowered to achieve safer recoveries and optimal aesthetic outcomes.
